Healthcare organizations generated 30% of the world’s data in 2025. 47% of this data is underutilized in clinical and business decision-making, even though four out of five healthcare leaders consider their data accurate. This gap between data generation and data-driven action costs the industry billions annually in missed diagnoses, operational waste, and revenue leakage.
The global healthcare analytics market was valued at $55.52 billion in 2025 and is on track to exceed $166 billion by 2030, growing at a 24.6% CAGR. Healthcare AI spending by providers alone hit $1.4 billion in 2025, with $600 million directed to ambient clinical documentation and $450 million to coding and billing automation.
Behind these numbers is a sector under immense financial and operational pressure. Clinician burnout is at crisis levels, with physicians spending 13 hours weekly on indirect patient care tasks. Claim denial rates above 10% have surged from 30% of providers in 2022 to 41% in 2025. And payers are now deploying AI to deny claims at a speed and scale that manual workflows cannot match.
The main question is not whether to invest in healthcare analytics, but where to invest to generate the fastest measurable return.
This article examines three high-impact areas where healthcare analytics is delivering proven results: patient outcomes, operational efficiency, and revenue cycle performance. We also outline the data infrastructure required to make analytics work across the enterprise.
Predictive analytics in healthcare: improving patient outcomes
Predictive analytics has become the fastest-growing segment in healthcare analytics, expanding at a 26.5% CAGR through 2030. The core value proposition is: use machine learning models to identify high-risk patients before their conditions escalate, enabling proactive interventions that reduce hospitalizations, readmissions, and mortality.
Early detection and risk stratification
Predictive models achieve substantially better accuracy when they incorporate social determinants of health (SDoH) alongside clinical data. Factors like housing stability, food security, transportation access, and income level have a measurable impact on patient outcomes.
Roughly half of hospital readmissions are rooted in social determinants, making them more influential than clinical comorbidity factors alone.
Kaiser Permanente integrated SDoH data into its IBM Watson Health predictive analytics platform alongside EHR and claims data, enabling identification of high-risk patients for targeted care plans that reduced hospitalizations and improved chronic disease management.
As health systems adopt value-based care models, the ability to layer SDoH data into analytics pipelines is becoming a competitive differentiator for population health management.
NYU Langone developed NYUTron, a large language model that examines physicians’ notes to predict patient outcomes, including 30-day rehospitalization risk with 80% accuracy.
At Mount Sinai, machine learning models developed during the COVID-19 pandemic analyzed patient history, vital signs, and lab results at admission to predict the likelihood of critical events such as intubation.
Blue Cross NC deploys ML to proactively identify members at risk of serious health events by analyzing patterns like missed follow-up visits and co-occurring conditions.
Healthcare systems deploying AI-based predictive analytics regularly report 10 to 20% reductions in readmission rates. UnityPoint Health achieved a 25% reduction using an AI clinical decision support tool, while Intermountain Healthcare documented a 15-20% reduction across units using AI-triggered intervention pathways. With unplanned readmissions costing the U.S. healthcare system roughly $26 billion annually, even a modest reduction translates to significant savings per institution.
Personalized treatment plans
Beyond risk stratification, machine learning models are enabling precision treatment planning by analyzing individual genetic profiles, clinical biomarkers, environmental factors, and lifestyle data to match patients with the therapies most likely to succeed.
In oncology, Tempus AI has built one of the largest multimodal clinical datasets in the industry, connecting molecular sequencing data with clinical records from more than 50% of U.S. oncologists.
The company’s PurIST algorithm helps clinicians select between first-line chemotherapy regimens for advanced pancreatic cancer based on tumor subtyping. Northwestern Medicine became the first health system to integrate Tempus’ generative AI clinical copilot directly into its EHR, enabling real-time, AI-driven treatment insights at the point of care.
In cardiovascular care, predictive models analyze individual risk factors against networks of similar patients to produce personalized risk projections, helping cardiologists tailor prevention strategies to each patient’s profile.
The shift toward AI-assisted treatment selection is significant because it addresses a core limitation of traditional evidence-based medicine: population-level trial data doesn’t account for individual patient variability.
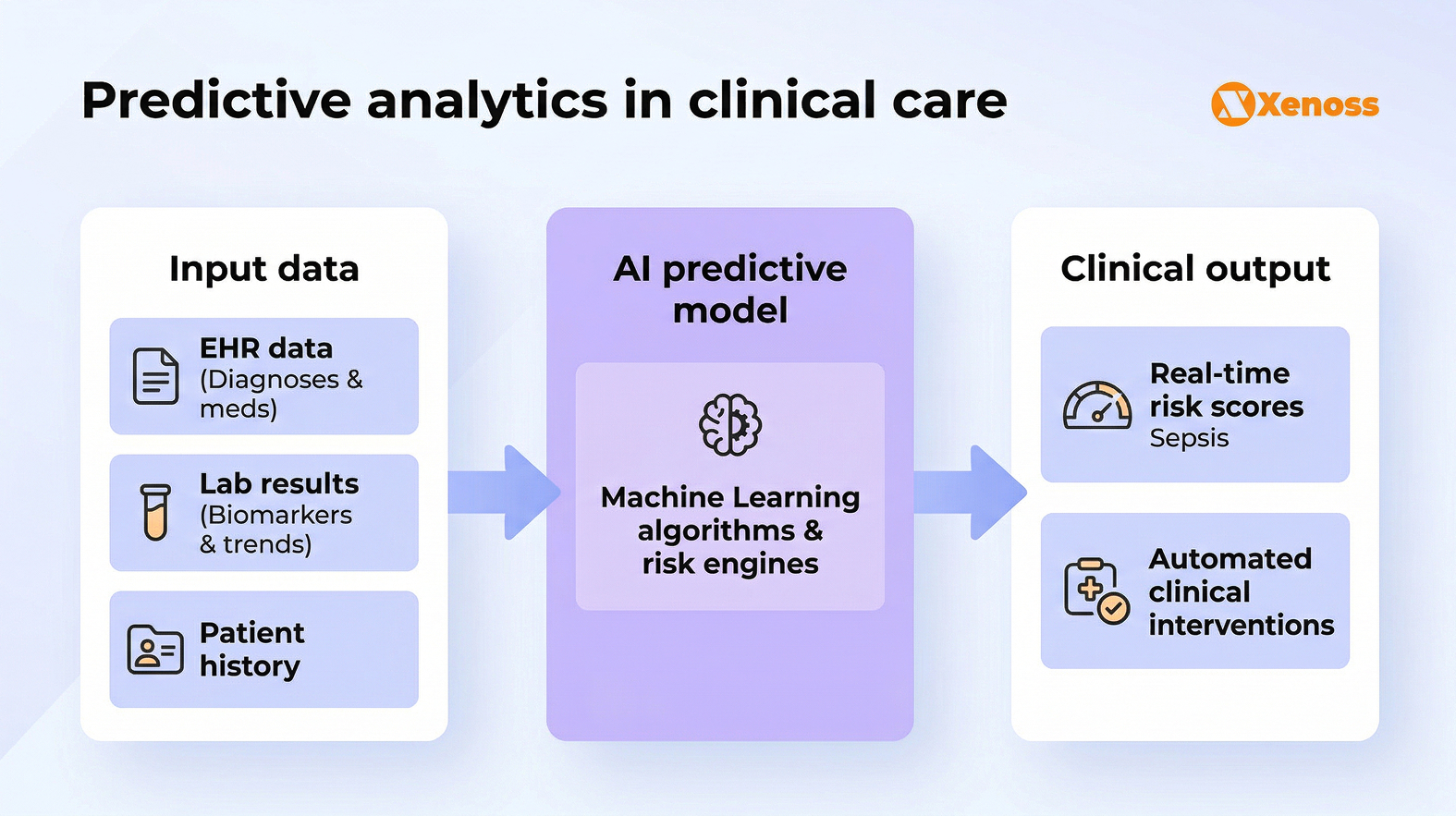
Healthcare analytics for operational efficiency
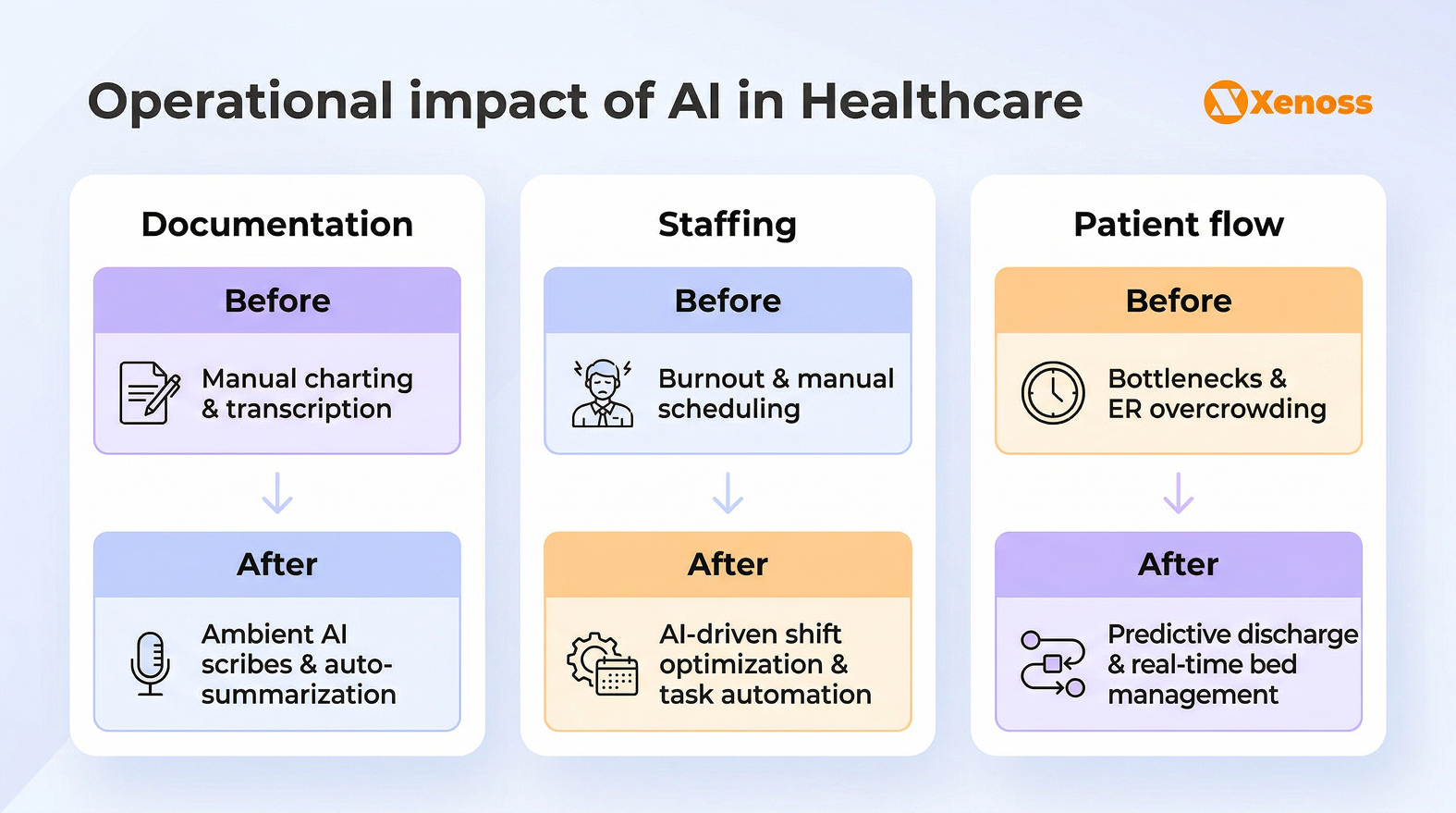
Operational inefficiencies cost the U.S. healthcare system over $250 billion annually in administrative complexity alone. Healthcare analytics targets the highest-waste areas: clinical documentation, staffing, scheduling, and resource allocation.
Ambient clinical documentation
Ambient AI scribes represent healthcare AI’s first breakout category. The segment generated $600 million in revenue in 2025, growing 2.4x year over year. 100% of health systems now report some usage of ambient clinical documentation tools, making it the most universally adopted AI use case.
The clinical evidence is compelling. A randomized trial conducted by UW Health and published in NEJM AI demonstrated that ambient AI notetaking reduced documentation time by 30 minutes per day per provider, improved diagnosis billing accuracy, and produced a clinically meaningful reduction in burnout scores. After the trial (August 2024 through March 2025), UW Health rolled out the system across clinics and hospitals in Wisconsin and Illinois.
Workforce optimization and resource allocation
AI-powered scheduling and staffing tools analyze historical patient flow data, seasonality, and real-time variables to optimize workforce deployment. Hospitals using these systems report improved bed turnover rates and staffing efficiency, directly reducing operational costs while maintaining care quality. Combined with data pipeline engineering that connects EHR systems, scheduling platforms, and staffing databases, health systems can create real-time visibility into operational bottlenecks.
Patient flow optimization, powered by real-time monitoring and predictive modeling, addresses one of the most persistent challenges in emergency departments.
AI systems can:
- Predict patient census levels
- Recommend optimal staffing ratios
- Identify discharge readiness
This reduces wait times and improves throughput. Hospitals deploying AI-driven patient flow tools can expect a 4% to 10% improvement in avoidable days and a 10% to 20% increase in resource utilization.
HonorHealth, for example, implemented a care operations automation system that achieved an 86% early discharge plan rate and saved $62 million by reducing excess patient days.
AI-powered revenue cycle management
Revenue cycle management is where healthcare analytics delivers the most immediate and quantifiable financial return. Health systems spend over $140 billion annually on revenue cycle operations. Nearly 20% of claims are denied on average, and as many as 60% of those denials are never appealed, representing millions in lost revenue per health system.
In 2025, more than 30% of providers prioritized AI and automation implementation for seven specific revenue cycle use cases, up from four to five use cases in previous years. 63% of providers have introduced AI into their RCM workflows, and according to a 2025 industry survey, 72% of executives report that their highest priority for revenue cycle investment is technology such as automation and AI.
Autonomous medical coding
Autonomous coding is one of the most mature AI applications in revenue cycle management. Natural language processing translates clinical notes into medical codes with high accuracy, reducing manual effort and coding errors.
Inova Health System: After implementing Nym’s autonomous medical coding engine, Inova achieved $1.3M in annual savings, a 50% decrease in weekly revenue sitting in DNFB, and a 10% increase in average charges per ED encounter.
Cleveland Clinic: The AI coding assistant can read a clinical document in less than two seconds and process more than 100 documents in 1.5 minutes.
Denial management in healthcare: prevention and recovery
AI-driven denial prevention uses predictive models trained on historical claims data and payer behavior to flag high-risk claims before submission.
Thoughtful AI: Healthcare organizations working with Thoughtful AI typically experience a 75% reduction in preventable denials, 80% decrease in operational costs, and up to 95% less manual work for RCM staff. AI Agents consistently perform at 95%+ accuracy.
Auburn Community Hospital, an independent 99-bed rural access hospital, uses robotic process automation, natural language processing, and machine learning in revenue cycle management. Over the years, Auburn has seen a 50% decrease in discharged-not-final-billed cases, a more than 40% improvement in coder productivity, and a 4.6% increase in case mix index. The overall impact on its bottom line was a little over $1 million, more than 10 times its investment.
Banner Health automated much of its insurance coverage discovery using a combination of a service that finds each patient’s coverage and a bot that adds that coverage to the patient’s account in various financial systems. A different bot handles insurance company requests for additional information. The health system also uses a bot to automatically generate appeal letters based on certain denial codes. Banner also developed its own predictive model that determines whether a write-off is warranted based on certain denial codes and the low probability of payment.
Healthcare financial analytics at scale
The healthcare financial analytics market grew from $9.74 billion in 2025 to $11.42 billion in 2026, at a 17.2% CAGR. This growth reflects the shift from treating the revenue cycle as a back-office function to managing it as a strategic asset.
AI-enhanced revenue operations create unified views of patient journeys from initial contact through billing and follow-up care, enabling organizations to identify bottlenecks, optimize conversion rates, and align clinical and business operations.
90% of healthcare leaders report that revenue cycle labor challenges exacerbate operations, with increasing denials costing hospitals over $20 billion annually and manual processes driving an average $25 rework cost per denied claim.
At scale, organizations that unify financial analytics across coding, billing, collections, and patient payments gain the ability to forecast cash flow, benchmark payer performance, and quantify the ROI of individual AI investments across the revenue cycle.
Healthcare analytics applications by category, maturity, and expected ROI
| Application area | Maturity level | Primary ROI driver | Typical results |
|---|---|---|---|
| Predictive patient risk scoring | Scaling | Reduced readmissions | 10-20% readmission reduction |
| Ambient clinical documentation | Widely adopted | Clinician productivity | 30 min/day saved per provider |
| Autonomous medical coding | Mature | Coding cost reduction | $500K+ annual savings |
| Denial prevention | Scaling | Revenue recovery | Up to 75% denial reduction |
| Patient flow optimization | Pilot phase | Operational efficiency | Up to 20% shorter stays |
How to build a healthcare data analytics platform
Deploying healthcare analytics at scale requires more than selecting AI tools. It demands a coherent data engineering strategy that addresses the unique challenges of healthcare data: strict regulatory requirements (HIPAA, GDPR, EU AI Act), diverse data types (structured EHR records, unstructured clinical notes, imaging data), and legacy system dependencies.
Healthcare data integration and interoperability
The foundation of any healthcare analytics initiative is a unified data layer. Health systems typically operate dozens of disconnected systems: EHRs, lab information systems, billing platforms, scheduling tools, and claims management software. Building interoperable data pipelines that connect these sources, using standards like HL7 FHIR, enables the cross-functional data access that analytics requires.
As Xenoss engineers have observed across enterprise implementations, 80% of success in AI projects comes from proper problem analysis and domain understanding. In healthcare, this means mapping clinical workflows, identifying where data quality breaks down, and building governance frameworks before deploying models. A rushed AI deployment on top of fragmented, low-quality data will fail, regardless of model sophistication.
Healthcare compliance and data security architecture
Healthcare data breaches cost an average of $7.42 million per incident in 2025, and organizations take 279 days to detect and contain one. Shadow AI, the use of unauthorized AI tools by staff without IT approval, is now present in 40% of hospitals. These risks make compliance-first architecture design a prerequisite for any analytics initiative.
A strong infrastructure includes encrypted data pipelines, role-based access controls, continuous monitoring, and audit trails that satisfy HIPAA and emerging AI-specific regulations. For organizations processing data across jurisdictions, the architecture must also address data residency requirements.
Technology stack decisions
Enterprise health systems face a critical choice between building custom analytics infrastructure and integrating vendor solutions. In Xenoss experience delivering custom AI solutions for Fortune 500 organizations, the most effective approach is typically hybrid: standardize on a core data platform for integration and governance, layer in best-of-breed AI models for specific use cases, and maintain the flexibility to swap components as the market evolves.
Key infrastructure components include a centralized data lake or lakehouse architecture, real-time streaming capabilities for clinical monitoring, robust MLOps processes for model training, deployment, and monitoring, and API-driven integration layers that connect analytics outputs to clinical workflows and EHR systems.
Risks and tradeoffs
Healthcare analytics adoption carries specific risks that organizations should evaluate before committing resources.
- Data quality dependency. AI models are only as reliable as the data they process. In healthcare, where clinical notes are often inconsistent, and EHR data is fragmented across systems, poor data quality leads to inaccurate predictions. Organizations should invest in data governance and quality monitoring before scaling analytics.
- Model generalizability. 60% of studies faced challenges with generalizability across diverse patient populations. A model trained on one hospital’s data may perform poorly at another due to differences in patient demographics, clinical practices, and coding conventions. Poor cross-site generalizability remains a major barrier to clinical deployment.
- Regulatory uncertainty. Healthcare AI governance is still evolving. The EU AI Act, FDA guidance on AI/ML-based software, and state-level AI privacy laws create a complex compliance landscape. Organizations need dedicated governance structures to keep pace.
- Change management. Technology adoption without cultural buy-in produces limited results. RCM leaders emphasize investing in change readiness, communication, and leadership capability alongside system deployments. 86% of revenue cycle leaders see value in AI, but only 44% of corporate leaders do, highlighting the internal alignment gap.
- Cost and timeline. Enterprise-grade healthcare analytics infrastructure requires significant upfront investment in data integration, compliance, and talent. Organizations should plan for 12 to 18-month implementation timelines for end-to-end analytics platforms, with a phased rollout starting from the highest-ROI use cases.
Bottom line
Organizations integrating AI across clinical workflows, revenue operations, and patient engagement are seeing measurable results: 30% efficiency gains, reduced readmissions, and millions recovered in previously lost revenue. The healthcare predictive analytics market alone is projected to reach $140 billion by 2035, driven by EHR volumes, value-based care mandates, and the growing sophistication of AI/ML models.
For health system leaders evaluating analytics investments, the clearest path to ROI starts with the use cases that address the most acute operational pain: ambient clinical documentation, autonomous coding, and denial prevention. From there, building toward a unified data engineering foundation enables the expansion into predictive patient analytics, population health management, and precision treatment planning.


